Pillar Procedure Alternatives
Non-Invasive Solutions for Snoring and Sleep Apnea
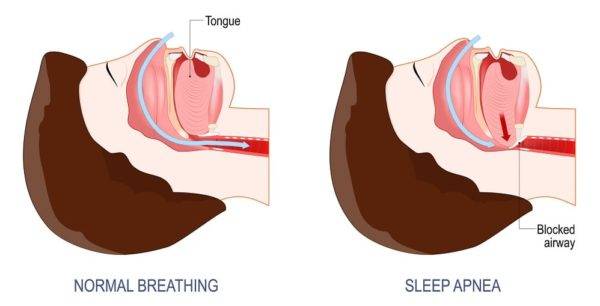
If you are one of the 18 million Americans looking for the best solution to snoring and obstructive sleep apnea, keep reading. CPAPs did not work. Losing weight did not work. You’re exhausted and concerned about long term risks.
Your next move was to try the pillar implant procedure, but now you’re stuck. As of right now, the pillar procedure is unavailable because the inserts used in the procedure are not currently being manufactured.
But there’s good news! New procedures work just as well (or better), with even less discomfort and less downtime. Let’s explore your alternatives and figure out which solution will work for you.
Comparison of Treatments for OSA and Snoring
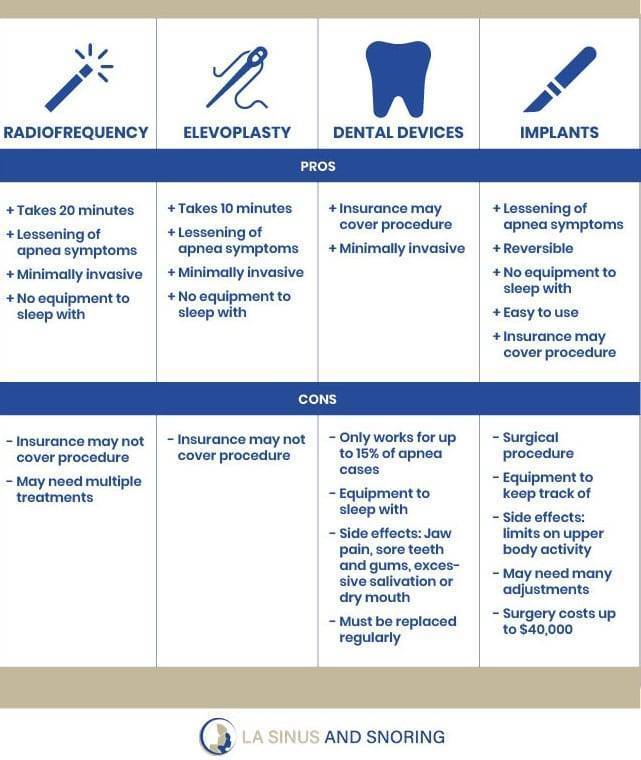
Maybe you’ve heard from your dentist that an oral appliance such as the mandibular advancement device (MAD) or tongue retaining device are a smart investment for your sleep.
Both of these oral devices work by targeting the placement of your tongue. This sounds great in theory, but only 10-15% of all snoring cases are linked to tongue placement.
The only way to know if you have a tongue obstruction is to meet with an ENT doctor and receive a diagnosis.
Pros of dental devices:
● Many patients find dental devices more comfortable than CPAP masks
● There is less equipment to knock off while sleeping
● Easier to travel with than CPAP
● Inexpensive; around $2,000 for device, visits, adjustments and follow-ups
● Most health insurance companies and Medicare cover oral devices for sleep apnea
Cons of dental devices:
● Only works if your OSA is caused by tongue placement
● Jaw pain, soreness, or tension
● Sore teeth and/or gums
● Excessive salivation or dry mouth
● Must be replaced regularly
In recent years, new obstructive sleep apnea implants have been approved by the FDA. Even more devices are in clinical trials to treat obstructive sleep apnea and chronic snoring.
INSPIRE
The Inspire OSA implant device — FDA approved since 2014 — has two leads. One senses your breathing in the intercostal muscle area. The other stimulates the hypoglossal nerve that controls key airway muscles to open your throat. Patients can turn on the implant using a remote control before bed and turn off upon awakening.
The procedure is minimally invasive and recovery time is short. Scarring may occur along the three incision points (under your chin, under the collarbone and on the side of your rib cage). The system should be checked by a doctor 1-2 times per year to confirm placement and functionality.
THN SLEEP THERAPY
The THN device — currently in trials — is placed near the hypoglossal nerve to deliver mild impulses to the tongue during sleep. It’s like a pacemaker for your tongue. A remote control can start, stop or pause the therapy, and also to recharge the implant.
The procedure is minimally invasive, with the implant inserted 4 cm below the clavicle. Recovery time is fast. Cost and insurance coverage are yet unknown.
NYXOAH GENIO SYSTEM
The Nyxoah Genio OSA implant device is working toward FDA approval. It is surgically inserted into the chin, and sits like a saddle on the genioglossus muscle, with electrodes facing the hypoglossal nerve. The stimulation to this nerve helps keep the upper airway open.
This implant is activated by a chip that the patient places at bedtime with a sticky patch. The chip needs to be charged daily.
Pros of implants:
- Patients report overall improvement in quality of life
- Unobtrusive; day-to-day activities and diet largely unaffected
- Low maintenance
- Completely reversible
- No tubes or unwieldy equipment to sleep with
- Easy to use, especially for those with disabilities
- Costs may be covered by insurance and Medicare
Cons of implants:
- Surgical procedure lasts hours; one-night hospital stay may be required
- Remotes can get lost if you have children or pets
- Potential limitations on strenuous upper body activity
- Inspire batteries aren’t rechargeable
- Expensive: Inspire costs up to $40,000 to place plus $17,000 for battery replacement
Like the pillar procedure, Elevoplasty and Radiofrequency (RF) treatments both stop airway obstruction caused by the soft palate.
Elevoplasty lifts the palate; RF stiffens the palate, and they both offer treatment without implants or inserts.
ELEVOPLASTY
This procedure lifts the soft palate, clearing the way for unobstructed breathing — and no snoring. The treatment can be performed in one office visit about 10 minutes. A doctor makes three small holes in the soft palate and places three resorbable sutures.
You can expect a sore throat for a few days after the treatment, but nothing over-the-counter pain medication couldn’t handle. Avoid spicy food until healed. Most patients report a decrease in snoring in just 30 days.
Pros of Elevoplasty:
- Takes 10 minutes
- Patients report decrease in snoring in 30 days
- Minimally invasive
- No tubes or unwieldy equipment to sleep with
Cons of Elevoplasty:
- May not be covered by insurance
RADIOFREQUENCY
This procedure stiffens the soft palate tissue that has a tendency to vibrate when you sleep, causing a snoring sound. RF can be performed by an ENT doctor under local anesthesia in less than 20 minutes. The doctor delivers a low-power, low-temperature treatment through a needle-tip wand.
While the tissue is healing in the days afterward, it stiffens. A few treatments may be needed for full benefits. Within four-six weeks, patients notice a big difference in snoring. In addition to the soft palate, RF can target turbinates in the nose and excessive tongue tissue to help breathing.
Pros of RF:
- Takes 20 minutes
- Patients report decrease in snoring in 4-6 weeks
- Minimally invasive
- No tubes or unwieldy equipment to sleep with
Cons of RF:
- May not be covered by insurance

Which non-invasive treatment for Snoring and OSA is best?
Not sure which of these alternatives to pillar and CPAP will prevent your soft palate from interfering with sleep? There’s no way to know until you learn what’s causing your snoring and/or sleep apnea.
Since the causes of snoring and sleep apnea are individual to each patient, Dr. Kayem will recommend procedures custom to your needs.
After a sleep study and diagnosis with Dr. Kayem, you’ll know the reason behind your snoring, and learn which minimally invasive procedure will best provide results.
